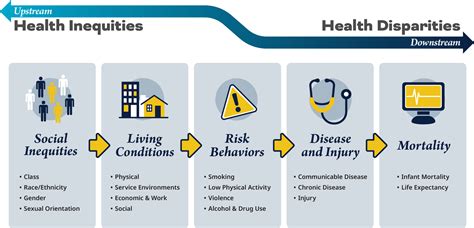
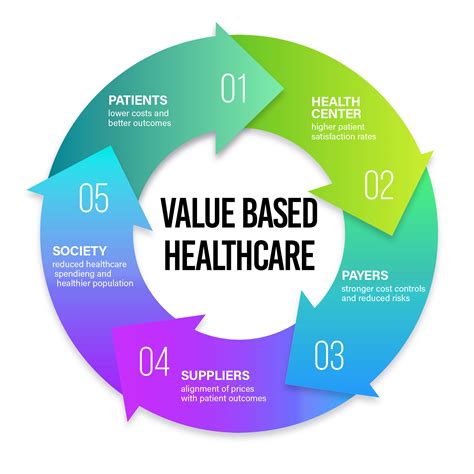
Health disparities in autoimmune disease have become a critical area of focus for researchers and healthcare professionals alike. These disparities manifest in various ways, including differences in disease incidence, prevalence, and outcomes across different demographic groups. This article explores the complexities of health inequities in autoimmune diseases, backed by evidence-based statements and real examples, and offers practical insights for stakeholders in the healthcare sector.
Key Insights
- Autoimmune diseases often show pronounced differences in incidence and severity among different racial and ethnic groups.
- Healthcare access and quality significantly influence the experience of autoimmune disease disparities.
- Targeted interventions and awareness campaigns can help reduce health disparities in autoimmune diseases.
Socioeconomic Factors Influencing Autoimmune Disease Outcomes
Socioeconomic factors play a crucial role in shaping the burden of autoimmune diseases. Individuals from lower socioeconomic backgrounds often face higher risks of developing autoimmune conditions, as well as poorer health outcomes. This is largely due to limited access to quality healthcare, inadequate health education, and suboptimal living conditions, which exacerbate disease management challenges. For example, research shows that African Americans with lupus tend to experience more severe symptoms and poorer prognoses compared to their Caucasian counterparts, partly due to socioeconomic disadvantages. To address this, it’s essential for healthcare providers to offer culturally sensitive care and integrate social determinants of health into their treatment plans.Racial and Ethnic Disparities in Autoimmune Disease Care
Racial and ethnic disparities in autoimmune disease care highlight systemic inequities in the healthcare system. Minority populations often receive less optimal care for autoimmune conditions, leading to worse health outcomes. A study found that Hispanic and African American patients with rheumatoid arthritis receive fewer disease-modifying antirheumatic drugs (DMARDs) compared to non-Hispanic whites, which can significantly affect disease progression and quality of life. This disparity is multifactorial, involving genetic, environmental, and socio-cultural elements. To bridge this gap, healthcare systems must implement equity-focused initiatives that include targeted education and outreach programs, and actively work towards dismantling systemic biases in healthcare delivery.FAQ Section
Why do health disparities exist in autoimmune diseases?
Health disparities in autoimmune diseases arise from a complex interplay of genetic, environmental, and socio-economic factors. Access to healthcare, education, and living conditions significantly impact disease onset and management.
How can we improve care for minority groups affected by autoimmune diseases?
To improve care, healthcare providers must adopt a culturally competent approach, ensuring equitable access to advanced treatments, regular monitoring, and comprehensive education tailored to the specific needs of minority populations.
In conclusion, addressing health disparities in autoimmune disease requires a multifaceted approach that encompasses better understanding of the underlying factors, enhancing healthcare access, and developing tailored interventions for affected populations. With concerted efforts from healthcare professionals, policymakers, and community organizations, we can strive towards a more equitable healthcare system for all.