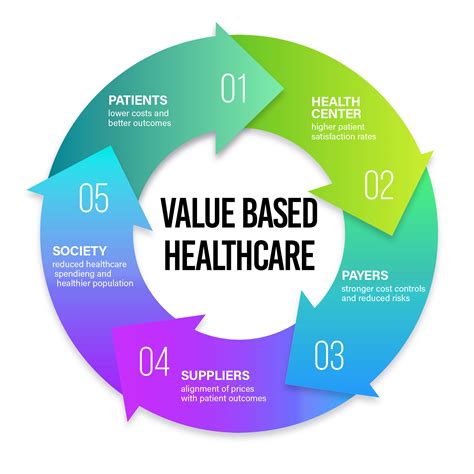
Welcome to our comprehensive guide on Value Based Care models provided by United Healthcare. Value Based Care is a healthcare system designed to improve the quality of care and patient satisfaction while reducing unnecessary costs. The goal is to deliver better health outcomes through a shift from traditional fee-for-service models to models that reward healthcare providers for the overall health of their patients rather than for the quantity of services rendered. United Healthcare has implemented several innovative Value Based Care models to achieve these objectives. This guide will provide you with step-by-step guidance to understand and implement these models effectively.
Understanding the Need for Value Based Care
In traditional healthcare systems, the focus often centers around volume rather than value, leading to excessive spending and not necessarily better patient outcomes. Many patients experience fragmented care and overtreatment. Value Based Care aims to solve these issues by prioritizing patient health and satisfaction.
For instance, imagine a scenario where a patient receives multiple treatments for a chronic condition without achieving long-term health improvements, leading to higher overall healthcare costs. Value Based Care models address this by ensuring that providers are incentivized to deliver comprehensive, coordinated care that focuses on the patient’s overall well-being.
Key Points to Start with Value Based Care
Quick Reference
- Immediate action item with clear benefit: Identify any existing gaps in care and patient communication.
- Essential tip with step-by-step guidance: Start by mapping out your current care delivery process and identifying areas for improvement.
- Common mistake to avoid with solution: Overlooking patient feedback in care planning; always integrate patient perspectives into your care delivery strategy.
Getting Started with United Healthcare Value Based Care Models
United Healthcare’s Value Based Care models are designed to drive better health outcomes and reduce costs. Below, we will explore some key models United Healthcare utilizes, including their implementation steps and practical examples.
1. The Shared Savings Program
The Shared Savings Program (SSP) is one of the cornerstones of United Healthcare’s Value Based Care initiative. In this program, healthcare providers enter into contracts with United Healthcare, where they share in the financial savings generated by reduced unnecessary care and improved patient outcomes.
Here’s how you can begin integrating the SSP into your practice:
- Step 1: Understand the program requirements. Familiarize yourself with the criteria, metrics, and reporting requirements.
- Step 2: Engage with a United Healthcare representative to discuss eligibility and how to participate in the program.
- Step 3: Implement best practices for patient care that align with the program’s goals, such as effective care coordination, preventive screenings, and regular follow-ups.
- Step 4: Leverage available resources such as educational webinars, toolkits, and coaching support provided by United Healthcare.
Example: A primary care physician who successfully reduces hospital readmissions for their patients by implementing a robust care management program may share in the savings generated, leading to both better patient outcomes and financial rewards.
2. The Patient-Centered Medical Home (PCMH) Model
The Patient-Centered Medical Home (PCMH) model aims to provide comprehensive, accessible, and coordinated care. United Healthcare's PCMH model rewards practices for providing high-quality, patient-centered care.
Here’s a detailed how-to guide for adopting the PCMH model:
- Step 1: Establish a team-based approach to care. Ensure your practice includes physicians, nurses, care managers, and other staff trained to work collaboratively.
- Step 2: Implement electronic health records (EHR) to facilitate better documentation and communication among care team members.
- Step 3: Invest in care coordination tools and patient engagement strategies, such as telehealth services and patient portals.
- Step 4: Measure and track key performance indicators (KPIs) such as patient satisfaction, care quality, and utilization metrics.
Example: A PCMH practice might use its EHR system to track patients’ chronic disease management and ensure they receive regular follow-ups, ultimately reducing emergency room visits and hospitalizations.
FAQ: Practical Application of Value Based Care Models
What are the biggest challenges in transitioning to a Value Based Care model?
One of the biggest challenges in transitioning to a Value Based Care model is the initial shift in mindset from volume to value. Practices often need to overhaul their existing workflows, adopt new technologies, and change how they measure success. Another challenge is the resistance from staff and patients accustomed to the traditional fee-for-service model. To address these challenges, it's essential to provide thorough training and education for your team, involve staff in the transition process to gain their buy-in, and clearly communicate the benefits of Value Based Care to both staff and patients.
3. The Bundled Payment Model
The Bundled Payment Model groups various services into a single payment. United Healthcare’s Bundled Payment Model seeks to improve coordination among providers and promote efficient care delivery.
To effectively implement this model:
- Step 1: Select the appropriate episode of care for bundled payments, such as joint replacement or heart failure management.
- Step 2: Assemble a care team that includes physicians, therapists, case managers, and others involved in patient care across different settings.
- Step 3: Develop a coordinated care plan that aligns with the goals of the bundled payment, focusing on reducing unnecessary services and improving patient outcomes.
- Step 4: Use data analytics and performance metrics to monitor care delivery and adjust strategies to achieve the best possible outcomes.
Example: A coordinated care team for a patient undergoing a total knee replacement might work together to ensure the patient receives preoperative education, postoperative physical therapy, and appropriate medication management to achieve a smooth recovery.
4. The Comprehensive Primary Care Plus (CPC+) Model
The Comprehensive Primary Care Plus (CPC+) Model offers primary care practices expanded resources and accountability for patient care across the entire health system.
Here’s how to integrate the CPC+ model into your practice:
- Step 1: Meet the eligibility requirements, which include providing comprehensive primary care services and committing to performance improvements.
- Step 2: Enroll in the CPC+ Model through United Healthcare’s program, and establish a detailed care plan with clear goals and metrics.
- Step 3: Enhance your care delivery by adopting evidence-based practices, integrating patient-centered approaches, and leveraging technology for better care coordination.
- Step 4: Engage in ongoing performance improvement activities supported by regular data reviews and feedback from United Healthcare.
Example: A primary care practice participating in CPC+ might use data analytics to identify patients at risk for adverse outcomes and proactively provide preventive care and management strategies.
Best Practices for Value Based Care
To achieve successful implementation and sustained improvement in patient outcomes, consider the following best practices:
- Focus on patient-centered care: Ensure that patient needs, preferences, and values guide all care decisions.
- Implement care coordination: Use multidisciplinary teams and technology to streamline care and enhance communication among providers.
- Invest in training and education: Provide continuous training for your staff to adapt to new practices and technologies.
- Utilize data and analytics: Leverage data to track performance, identify areas for improvement, and measure outcomes.
- Engage patients actively: Involve patients in their care plans and provide them with the tools and information they need to manage their health effectively.
In conclusion, Value Based Care models by United Healthcare offer innovative approaches to improve healthcare delivery and patient outcomes. By adopting these models, healthcare providers can transition from a volume-based to a value-based system, ultimately leading to better patient care and reduced costs. Whether through the Shared Savings Program, the Patient-Centered Medical Home model, the Bundled Payment Model, or the Comprehensive Primary Care Plus model, United Healthcare provides the resources and support necessary to make this transition successful. This guide offers actionable advice and practical examples to help you navigate and implement these value-based models effectively.