Welcome to this comprehensive guide on key developments in Electronic Health Records (EHR) healthcare evolution. This guide is designed to provide step-by-step guidance with actionable advice, addressing the most pressing user pain points in EHR adoption and utilization. We’ll walk through the transformation journey from basic setup to advanced optimization, integrating practical examples and expert tips throughout.
Understanding the Need for EHR Evolution
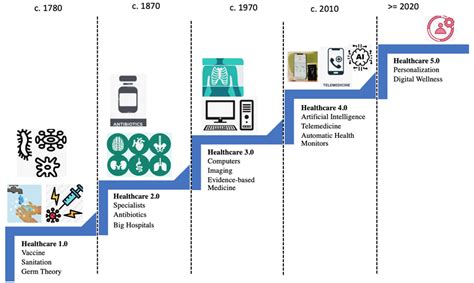
The healthcare landscape is continuously evolving, necessitating efficient, secure, and comprehensive patient management systems. The traditional paper-based healthcare systems have become cumbersome, inefficient, and error-prone. This guide aims to address the pressing need for robust Electronic Health Records (EHR) solutions that streamline patient care, enhance data accuracy, and foster better communication among healthcare providers.
Healthcare professionals today face numerous challenges: data silos, fragmented care records, and significant administrative burdens. Transitioning to an EHR system is not just about upgrading technology; it’s a transformative leap that can significantly improve patient outcomes, operational efficiency, and overall healthcare quality.
Quick Reference
Quick Reference
- Immediate action item: Conduct a thorough assessment of your current systems to determine the most appropriate EHR system that aligns with your needs.
- Essential tip: Ensure that your EHR system includes robust patient privacy and data security features, such as HIPAA compliance and encryption.
- Common mistake to avoid: Underestimating the importance of user training and engagement during the transition to EHR to maximize system utilization and minimize resistance.
Choosing the Right EHR System
Selecting the right EHR system is crucial for ensuring that your healthcare practice reaps maximum benefits from this technological investment. Here’s a step-by-step guide to making an informed decision.
1. Assess Your Current Workflow and Requirements
Before selecting an EHR system, evaluate your current workflow processes and determine what specific functionalities your practice requires. Key areas to consider include:
- Clinical functionalities: Does the EHR support necessary clinical workflows like electronic prescribing, patient charting, and medical billing?
- Interoperability: Is the system capable of integrating seamlessly with other healthcare systems and third-party applications?
- Customizability: Can the system be customized to meet the unique needs of your practice?
2. Evaluate Vendor Reputation and Support
Research the reputation of potential EHR vendors. Look for:
- Client testimonials: Read reviews from other healthcare providers to gauge their satisfaction with the system.
- Customer support: Ensure the vendor offers robust customer support, including 24⁄7 technical assistance.
3. Consider Cost and ROI
While it’s tempting to opt for the most affordable option, consider the long-term cost and return on investment (ROI). Look for:
- Initial investment: The upfront cost of purchasing the system.
- Implementation fees: Costs associated with installation, customization, and training.
- Ongoing costs: Monthly or annual subscription fees, maintenance, and support costs.
Evaluate how the system will help reduce operational costs and improve efficiency over time to ensure the ROI justifies the initial investment.
4. Review Certification and Compliance
Ensure that the EHR system is certified by a recognized body like the ONC-ATCB (Office of the National Coordinator for Health Information Technology - Accredited Certification Body) and complies with essential regulations, such as:
- HIPAA: Ensuring patient privacy and data security.
- MACRA: Promoting value-based care through quality reporting and performance metrics.
Implementation and Training
Successful implementation and training are vital to maximizing the benefits of your EHR system. This section provides a detailed guide on ensuring a smooth transition.
1. Develop a Detailed Implementation Plan
Creating a comprehensive implementation plan helps ensure a seamless transition. Consider the following steps:
- Data migration: Plan for transferring existing patient records to the new system. Validate data integrity and ensure that all historical data is correctly migrated.
- User training: Develop a training program that covers all aspects of the new system. Schedule training sessions well in advance and provide ample time for hands-on practice.
- Timeline: Establish a realistic timeline for implementation, accounting for all necessary preparations and training sessions.
2. User Training and Engagement
Effective training ensures that all users are proficient in using the EHR system. Here are some key strategies:
- Tailored training: Offer training sessions that are tailored to different user roles, such as doctors, nurses, and administrative staff.
- Hands-on practice: Provide ample opportunities for users to practice using the system in a safe environment before going live.
- Ongoing support: Establish a system for ongoing support and continuous learning to address new functionalities and updates.
Engaging users from the beginning helps to build trust and ensures that they become advocates for the new system.
3. Monitor and Optimize the System
Once the EHR system is live, continuous monitoring and optimization are essential for maximizing its benefits. Consider these steps:
- Feedback loops: Collect regular feedback from users to identify any pain points or areas for improvement.
- Performance metrics: Track key performance metrics, such as user satisfaction, system uptime, and data accuracy.
- Regular updates: Stay informed about updates and new features from the vendor and implement them as necessary.
Practical FAQ
What are the common challenges faced during EHR implementation?
Several challenges can arise during EHR implementation:
- Data migration issues: Ensuring accurate and complete transfer of patient records can be challenging.
- User resistance: Some staff may be resistant to adopting new systems, especially if they are comfortable with existing workflows.
- Training complexities: Providing comprehensive and effective training to all users can be time-consuming and may require additional resources.
- Integration problems: Seamlessly integrating the EHR system with existing infrastructure and third-party applications can present technical hurdles.
Proactive planning, comprehensive training, and ongoing support can help mitigate these challenges.
How can small practices ensure they get the best value from their EHR investment?
Small practices can maximize the value of their EHR investment by:
- Prioritizing essential features: Focus on implementing functionalities that are most critical to your practice, such as core clinical features and billing.
- Engaging in continuous learning: Encourage staff to participate in ongoing training and professional development to fully utilize the system’s capabilities.
- Regularly reviewing performance: Monitor key performance indicators to identify areas for improvement and ensure the system meets your evolving needs.
- Leveraging vendor support: Take advantage of vendor resources, including support, training materials, and user forums, to enhance system usage.
By focusing on these strategies, small practices can ensure that their EHR system delivers substantial benefits.
Advanced Optimization and Future Trends
Once your EHR system is fully implemented and optimized, exploring advanced optimization strategies and staying updated on future trends can help ensure your practice remains at the forefront of healthcare technology.
1. Advanced Analytics and Reporting
Leverage advanced