Home health care has emerged as an increasingly pivotal component of modern healthcare delivery, providing personalized services to individuals in the comfort of their homes. The significance of home health care is underpinned by its capacity to deliver high-quality, patient-centered care at a fraction of the cost associated with traditional hospital or facility-based care. This shift has not only been driven by advances in medical technology but also by an evolving understanding of the importance of patient satisfaction and recovery outcomes.
In light of its rising prominence, understanding home health care costs becomes a critical factor for policymakers, insurers, and patients alike. This article delves into the multifaceted nature of home health care expenses, offering practical insights, evidence-based statements, and real-world examples to clarify this vital subject.
Key Insights
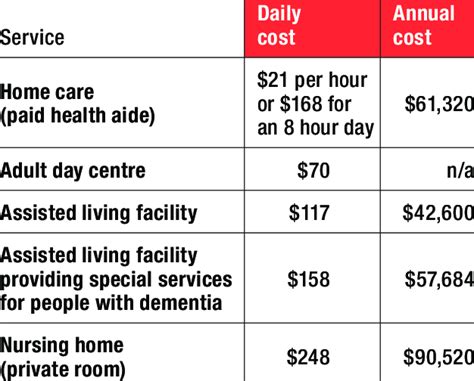
- Home health care costs can vary significantly based on the type of care required and patient needs.
- Reimbursement policies from Medicare and Medicaid play a pivotal role in managing home health care expenses.
- Investing in home health care can lead to substantial savings in the long term by reducing hospital readmission rates.
Factors Influencing Home Health Care Costs
The cost of home health care is influenced by a myriad of factors, each contributing uniquely to the overall expense. Primarily, the nature and intensity of the care required dictate the financial outlay. For instance, patients needing frequent skilled nursing visits will incur higher costs than those requiring intermittent physical therapy. Additionally, the geographical location plays a significant role; urban areas typically have higher labor costs, thereby driving up home health care expenses.
Another important consideration is the type of services provided. Home health care can include a broad spectrum of services ranging from skilled nursing care, therapy services, to medical social services. Each of these services has its own set of costs, influenced by the level of expertise required and the frequency of visits. For example, a skilled nurse might charge a different fee compared to a physical therapist due to the differing scopes of their expertise.
Impact of Insurance Coverage on Home Health Care Costs
Insurance coverage, particularly from government programs like Medicare and Medicaid, is a major determinant of home health care costs. These programs have established reimbursement rates that significantly influence the financial dynamics of home health care providers. For example, Medicare has introduced Home Health Prospective Payment System (HH PPS), which bundles payments for episodes of care, thereby controlling costs while ensuring adequate service delivery.
From an insurer’s perspective, the coverage policies help mitigate the escalating costs associated with traditional hospital care. For patients, understanding their insurance coverage can lead to more cost-effective care management. Typically, Medicare covers home health care if a doctor certifies that the patient is homebound, requires intermittent skilled nursing care, or needs part-time or intermittent skilled therapy.
Does Medicare cover all aspects of home health care?
Medicare covers a range of home health care services, including skilled nursing care, physical therapy, speech-language pathology services, occupational services, medical social services, and part-time or intermittent home health aide services, but it does not cover non-medical services like bathing and dressing.
Are there any out-of-pocket costs for home health care under Medicare?
Yes, while Medicare does cover many home health services, beneficiaries might still have to pay a coinsurance fee or deductible for certain services. It's important to review the specific plan details to understand potential out-of-pocket costs.
To summarize, home health care costs are shaped by a complex interplay of care requirements, geographical location, and insurance coverage. The evolving landscape of home health care is driven by both the need for cost-effective care solutions and the desire to enhance patient outcomes. By leveraging understanding of these factors, stakeholders can better navigate the economic considerations associated with this essential service.