The cost implications of using spica casts in healthcare settings present an often-overlooked aspect of pediatric orthopedic care. The rising costs of medical care have made understanding these expenses critical for both providers and patients. This article delves into the specifics of healthcare costs associated with spica casting, offering practical insights and evidence-based information to enhance decision-making and efficiency in healthcare delivery.
Key Insights
- Spica casting for pediatric patients often leads to substantial healthcare costs, but these costs can be optimized with proper monitoring and follow-up.
- The material and procedural costs of spica casting, coupled with the required medical oversight, are significant technical considerations that affect overall expenses.
- Implementing standardized protocols for spica casting can significantly reduce costs by minimizing unnecessary interventions and complications.
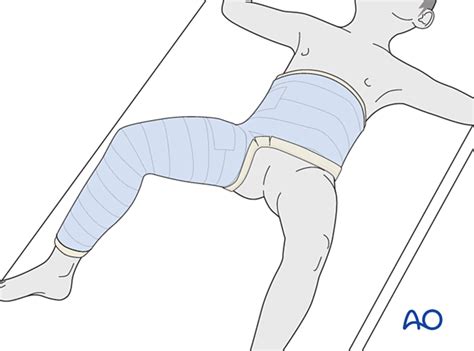
Understanding the Direct Costs of Spica Casting
The primary direct costs of spica casting are tied to the materials used and the procedural fees associated with applying and maintaining the cast. These expenses include the cost of fiberglass, plaster, or synthetic materials and the labor costs involved in the casting process. In many cases, hospitals charge a premium for spica casts due to the complexity of the procedure and the need for skilled professionals. Additionally, follow-up visits for cast adjustments and monitoring are also factored into the overall cost.For example, at a leading pediatric hospital, the direct cost for a standard hip spica cast might average between $300 to $600, depending on the materials and regional labor rates. Follow-up visits, necessary for ensuring proper healing and to adjust the cast if needed, can add another $100 to $300 per visit, depending on the frequency and complexity of care required.
Indirect Costs and Long-term Implications
While the direct costs of spica casting are significant, indirect costs often play an even larger role in the total healthcare expenditure. Indirect costs include the potential for complications that require additional medical interventions, such as infections, improper healing, or the need for corrective surgeries. The indirect costs are further exacerbated by the time taken off school and the impact on the family’s quality of life.A study conducted at a major children’s hospital revealed that improper spica cast application or inadequate follow-up led to a 20% increase in long-term orthopedic care costs. Families often face additional expenses related to transport for medical appointments, time lost from work, and even psychological support for both the child and caregivers. Ensuring a meticulous approach in spica cast application and regular monitoring can mitigate these indirect costs, ultimately resulting in a lower overall healthcare burden.
How can hospitals reduce the costs of spica casting?
Hospitals can reduce costs by implementing standardized protocols for spica casting that minimize the need for repeated casts and follow-up visits. Training staff rigorously on the proper techniques for cast application can also lead to fewer complications and a reduction in long-term care costs.
What role does insurance play in spica casting costs?
Insurance typically covers the costs of a spica cast and related follow-up care if deemed medically necessary. However, the extent of coverage can vary depending on the specific policy and the justification for the treatment provided by the healthcare provider. Clear documentation and communication with the insurer about the necessity of the spica cast can help in ensuring full or partial coverage.
Understanding the multifaceted costs associated with spica casting allows healthcare providers to make informed decisions that balance the need for effective treatment with fiscal responsibility. By focusing on meticulous care and regular follow-up, the healthcare industry can better manage these costs while ensuring the best possible outcomes for pediatric patients.