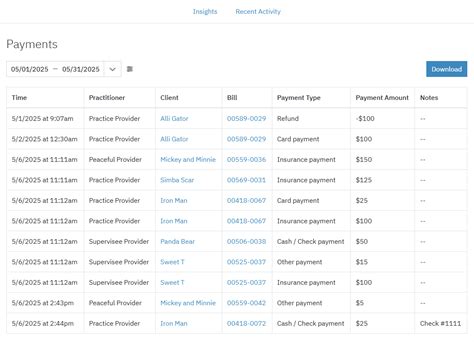
Pinning down the intricacies of client insurance payments within the health sector can seem daunting. Yet, understanding this facet is pivotal for any healthcare provider aiming for sustainable, seamless operations. This article delves into the fundamental principles of navigating this complex area, underpinned by practical insights and real-world examples to ensure clarity and actionable outcomes.
Key Insights
- Understanding the nuanced requirements for client insurance payments is crucial for avoiding financial pitfalls.
- Ensuring compliance with the latest health insurance regulations can prevent legal repercussions.
- Implementing a robust electronic health records (EHR) system enhances efficiency and accuracy in insurance processing.
Understanding the complexities of client insurance payments in healthcare involves more than just processing claims; it demands a comprehensive understanding of insurance policies, provider networks, and compliance with federal regulations. The significance of these elements cannot be overstated. A provider’s adherence to regulatory standards, such as those set by the Health Insurance Portability and Accountability Act (HIPAA), not only ensures legal compliance but also maintains patient trust and satisfaction.
For example, one prominent hospital chain implemented a stringent compliance checklist, which was integrated into their existing EHR system. By doing so, they ensured that all claims were processed accurately and in compliance with regulatory requirements, thus preventing fines and legal issues. This move also streamlined operations, reducing the administrative burden on their billing department.
In addition to regulatory compliance, understanding the intricacies of client insurance payments involves leveraging technology effectively. Modern electronic health records (EHR) systems have revolutionized how healthcare providers handle insurance claims and payments. These systems offer real-time data access, automated claim submissions, and detailed reporting, all of which significantly reduce the margin for error in insurance processing.
Consider a midsize clinic that adopted an advanced EHR system equipped with automated claim submission and payment tracking capabilities. This not only reduced the time spent on claim processing but also enhanced accuracy, resulting in fewer rejected claims and delayed payments. This improvement ultimately led to a healthier cash flow and better patient satisfaction rates.
Another crucial aspect is the role of provider networks in client insurance payments. Insurance companies often have specific networks of preferred providers, and understanding these networks is vital for maximizing reimbursement rates. Providers must ensure that they are in-network to avoid the complexities and delays associated with out-of-network claims.
For instance, a smaller private practice found that many of their claims were being denied because they were unaware that they had fallen out of an insurer’s network. By actively managing their network relationships and regularly updating their status with insurers, they were able to reverse this trend and ensure that most of their claims were processed without complications.
What are the common pitfalls in handling client insurance payments?
Common pitfalls include non-compliance with regulatory standards, errors in claim submission due to outdated software, and lack of understanding of insurer networks. These issues can lead to denied claims, delayed payments, and legal complications.
How can healthcare providers improve their efficiency in insurance processing?
Healthcare providers can improve efficiency by implementing advanced EHR systems, ensuring strict compliance with regulatory standards, and actively managing their provider networks. These steps help in reducing errors, improving reimbursement rates, and maintaining a healthy cash flow.
By meticulously addressing the key insights and implementing the recommended strategies, healthcare providers can navigate the complex landscape of client insurance payments with greater ease, ensuring financial stability and operational efficiency.